Efficacy of Modified Periarticular Infiltration Compared with Conventional Periarticular Infiltration in Controlling Pain After Total Knee Arthroplasty: A Randomized Controlled Non-Inferiority Trial
DOI:
https://doi.org/10.56929/jseaortho-2026-0290Keywords:
conventional periarticular infiltration, multimodal analgesia, modified periarticular infiltration, morphineAbstract
Purpose: Patients with end-stage knee osteoarthritis typically undergo total knee arthroplasty (TKA), a surgical procedure that has long been considered a cost-effective treatment. However, moderate to severe postoperative pain is a common problem following TKA. Therefore, in this study, we aimed to compare the effects of postoperative pain management using conventional periarticular infiltration (conventional periarticular infiltration [PA]) versus modified periarticular infiltration (modified PA).
Methods: This study was designed as a randomized controlled non-inferiority clinical trial conducted from April 2024 to April 2025. A total of 58 patients undergoing primary unilateral TKA were enrolled and randomly assigned to receive either modified PA or conventional PA. The primary outcome was postoperative pain within the first 24 h after surgery, measured using the visual analog scale. Secondary outcomes included time to first morphine hydrochloride rescue, total morphine consumption during the first 24 postoperative hours, and length of hospital stay (LOS).
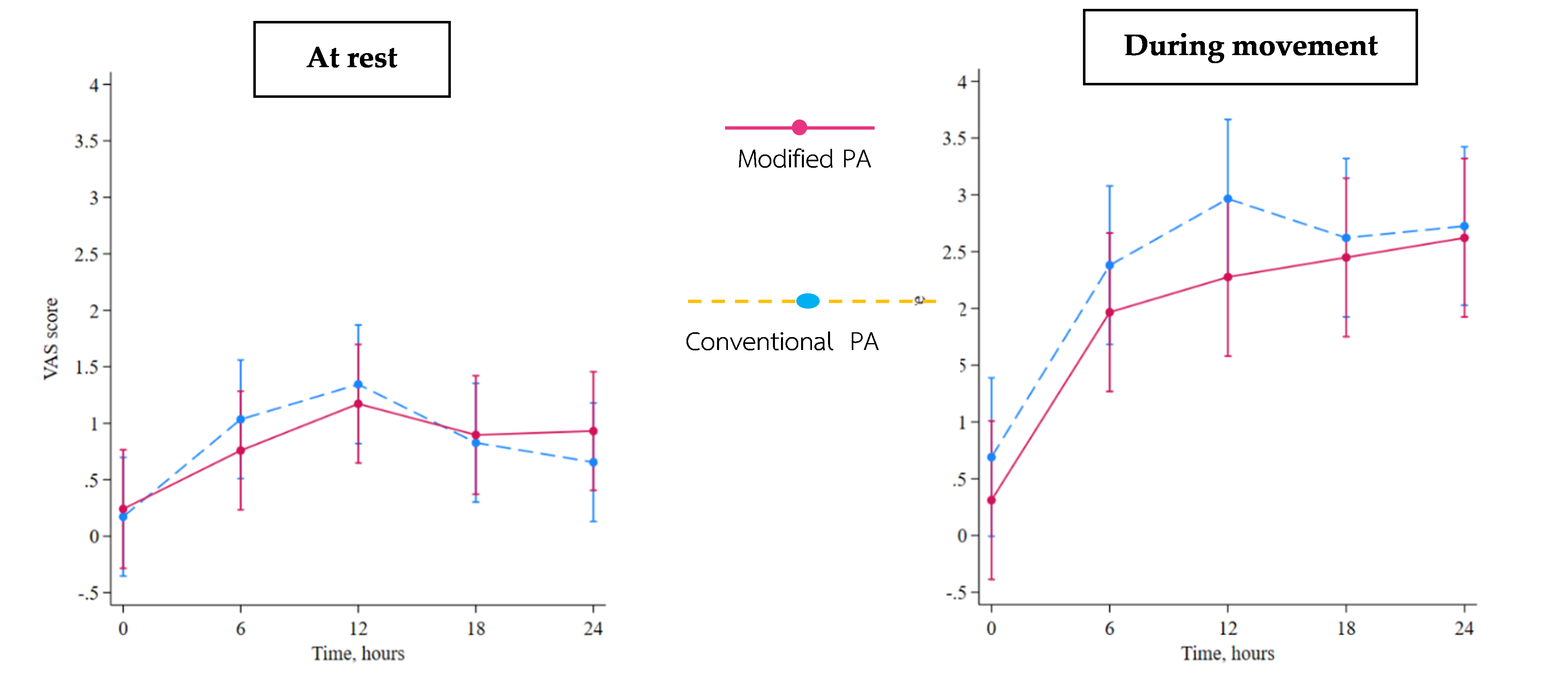
Results: Modified PA was non-inferior to conventional PA for postoperative pain control at rest and during movement within 24 h after TKA. Time to first morphine rescue, 24 h morphine consumption, and LOS did not differ significantly between the groups. All mean differences and corresponding 95% confidence intervals remained within the predefined non-inferiority margin of 0.5.
Conclusions: Modified PA and conventional PA provided comparable pain relief during the first 24 h after TKA and showed similar times to first morphine rescue. Morphine consumption and LOS were similar between the groups. These findings may inform the selection of intraoperative analgesic infiltration techniques.
Metrics
References
Karam JA, Schwenk ES, Parvizi J. An update on multimodal pain management after total joint arthroplasty. J Bone Joint Surg Am 2021;103:1652-62.
Jiang X, Wang QQ, Wu CA, et al. Analgesic efficacy of adductor canal block in total knee arthroplasty: A meta-analysis. Orthop Surg 2016;8:294-300.
Seangleulur A, Vanasbodeekul P, Prapaitrakool S, et al. The efficacy of local infiltration analgesia in the early postoperative period after total knee arthroplasty: a randomized, double-blind, placebo-controlled study. Eur J Anaesthesiol 2016;33:816-31.
Zuo W, Guo W, Ma J, et al. Does adductor canal block combined with local infiltration analgesia have a synergistic effect than adductor canal block alone in total knee arthroplasty: A meta-analysis and systematic review. J Orthop Surg Res 2019;14:101.
Sardana V, Burzynski JM, Scuderi GR. Adductor canal block or local infiltrate analgesia for pain control after total knee arthroplasty: A randomized controlled trial. J Arthroplasty 2019;34:183-9.
Tsai YF, Lin YC, Hsieh PH, et al. Incidence of local anesthetic systemic toxicity in patients receiving bupivacaine infiltration analgesia for total joint arthroplasty under general anesthesia: A retrospective single-center study. BMC Anesthesiol 2024;24:422.
Kuthiala G, Chaudhary G. Ropivacaine: A review of its pharmacology and clinical use. Indian J Anaesth 2011;55:104-10.
Hannon CP, Fillingham YA, Spangehl MJ, et al. Periarticular injection in total joint arthroplasty: The clinical practice guidelines of the American Association of Hip and Knee Surgeons, American Society of Regional Anesthesia and Pain Medicine, American Academy of Orthopaedic Surgeons, Hip Society, and Knee Society. J Arthroplasty 2022;37:1701-7.
Kerr DR, Kohan L. Local infiltration analgesia: a technique for the control of acute postoperative pain following knee and hip surgery: A case study of 325 patients. Acta Orthop 2008;79:174-83.
Nair VS, Radhamony NG, Rajendra R, et al. Effectiveness of intraoperative periarticular cocktail injection for pain control and knee motion recovery after total knee replacement. Arthroplasty Today 2019;5:320-4.
Van Erp JH, Keijser LC, van Haelst IM, et al. A patient with neurological and cardiac complications after local infiltration analgesia for total knee arthroplasty. Ned Tijdschr Orthop 2018;25:119-22.
Perret M, Fletcher P, Firth L, et al. Comparison of patient outcomes in periarticular and intraarticular local anaesthetic infiltration techniques in total knee arthroplasty. J Orthop Surg Res 2015;10:119.
Su C, Liu Y, Wu P, et al. Comparison between periarticular analgesia versus intraarticular injection for effectiveness and safety after total knee arthroplasty. J Perianesth Nurs 2022;37:952-5.
Mortazavi SMJ, Vosoughi F, Yekaninejad M, et al. Comparison of the effect of intra-articular, periarticular, and combined injection of analgesics on pain following total knee arthroplasty: a double-blinded randomized clinical trial. JB JS Open Access 2022;7:e22.00074.
Cheng KY, Feng B, Peng HM, et al. The analgesic efficacy and safety of periarticular injection versus intra-articular injection in one-stage bilateral total knee arthroplasty: a randomized controlled trial. BMC Anesthesiol 2020;20:2.
Laoruengthana A, Rattanaprichavej P, Rasamimongkol S, et al. Intra-articular tranexamic acid mitigates blood loss and morphine use after total knee arthroplasty: a randomized controlled trial. J Arthroplasty 2019;34:877-81.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 The Royal College of Orthopaedic Surgeons of Thailand

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






